Over half of all adults aged 65 and older report chronic difficulty initiating or maintaining sleep, according to the National Institutes of Health. If you find yourself staring at the ceiling at 3 a.m. or waking up utterly exhausted, your body is sending a clear signal that something in your routine needs to change. As you age, your natural sleep architecture shifts. You spend less time in the deep, restorative stages of sleep and more time in lighter stages, making you far more susceptible to nighttime disruptions.
However, chronic insomnia is not an inevitable consequence of getting older. It is a highly treatable condition that responds beautifully to targeted lifestyle adjustments and proper medical care.
“The most important investment you can make is in yourself.” — Warren Buffett
Investing time and effort into improving your sleep pays massive dividends for your physical health, cognitive function, and daily energy levels. Better rest even sharpens your financial decision-making and reduces healthcare costs over time. Below, we explore ten highly actionable strategies to help you reclaim your nights, ranging from simple bedroom adjustments to maximizing your Medicare benefits for sleep-related care.

10 Actionable Strategies for Restful Sleep
1. Anchor Your Wake-Up Time
Your circadian rhythm—the internal clock that dictates when you feel tired and when you feel alert—thrives on strict consistency. Going to bed and waking up at wildly different times confuses this biological clock. To fix this, establish a rigid wake-up time and stick to it seven days a week. Even if you experience a terrible night of sleep, force yourself out of bed at your anchored time. This builds healthy sleep drive throughout the day, ensuring you feel genuinely tired by the time your head hits the pillow the following night.
2. Optimize Your Bedroom Environment
A sleep-conducive environment is cool, dark, and quiet. As you age, your core body temperature changes, making you more sensitive to ambient heat. Aim to keep your bedroom thermostat between 60 and 67 degrees Fahrenheit. Install blackout curtains to block ambient streetlights, which can interfere with your brain’s melatonin production. If neighborhood noise or a snoring partner keeps you awake, invest in a white noise machine or a simple pair of silicone earplugs to block out sudden sounds.
3. Get Screened for Sleep Apnea
Obstructive Sleep Apnea (OSA) is incredibly common among older adults. It causes your airway to collapse during sleep, briefly cutting off your oxygen supply and forcing your brain to wake you up—sometimes dozens of times per hour. If you snore loudly, wake up gasping for air, or feel fatigued despite spending eight hours in bed, ask your doctor for a sleep study.
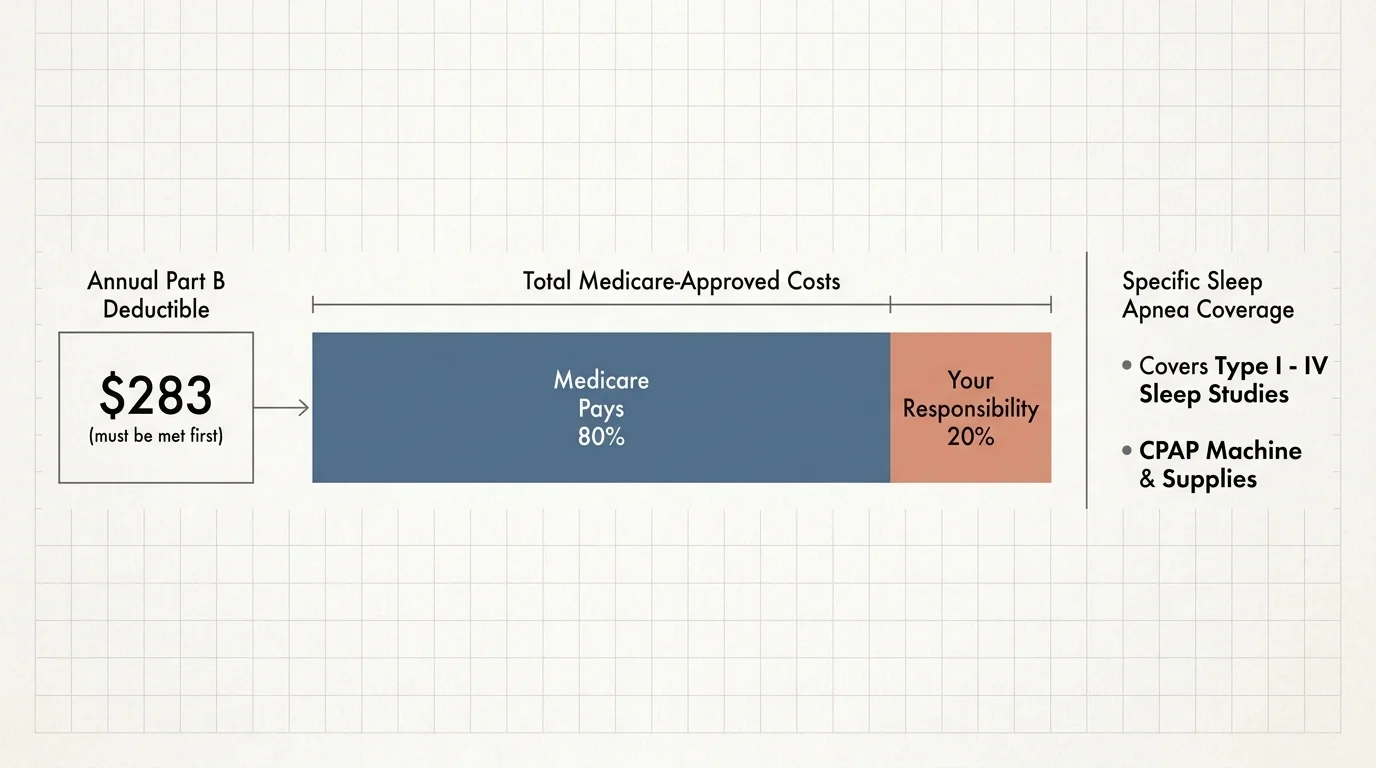
If you are worried about the cost of testing and equipment, rest assured that Medicare Part B provides robust coverage for sleep apnea. Once you meet your annual Part B deductible (which is $283 in 2026), Medicare covers 80% of the approved cost for Type I through IV sleep studies. If you are diagnosed with OSA, Medicare also covers 80% of the cost of a Continuous Positive Airway Pressure (CPAP) machine and its necessary supplies. You can review the exact coverage criteria directly on Medicare.gov.
4. Review Your Medications with Your Doctor
Polypharmacy—the use of multiple medications simultaneously—is a leading culprit behind senior insomnia. Many common prescriptions disrupt sleep architecture. For example, beta-blockers prescribed for high blood pressure can suppress nighttime melatonin production, while diuretics prescribed for fluid retention will cause frequent trips to the bathroom throughout the night. Schedule a comprehensive medication review with your primary care physician or pharmacist. Sometimes, simply shifting a morning pill to the evening, or vice versa, can drastically improve your sleep quality.
5. Manage Financial Stress to Quiet Your Mind
Financial anxiety is a notorious sleep thief. Lying awake worrying about taxes, inflation, or retirement account balances triggers a cortisol release that makes deep sleep impossible. Taking concrete steps to organize your finances provides profound mental relief.
For example, simply understanding your tax advantages can alleviate stress. For tax year 2026, the IRS provides a generous standard deduction of $16,100 for single filers and $32,200 for married couples filing jointly. Furthermore, taxpayers aged 65 and older receive an additional standard deduction of $2,050 for single filers and $1,650 per qualifying spouse for joint filers. Recent tax legislation also introduced a temporary $6,000 Senior Deduction per eligible person available through 2028. Knowing that these federal tax breaks protect a large portion of your income can help quiet your mind before bed. For the most current tax forms and bracket details, always consult the Internal Revenue Service (IRS).
6. Limit Late-Day Caffeine and Alcohol
As your metabolism slows with age, your body takes much longer to process caffeine. A cup of coffee consumed at 3:00 p.m. can still be actively blocking sleep receptors in your brain at 11:00 p.m. Switch to decaffeinated beverages or herbal teas after lunchtime.
Similarly, while a glass of wine might help you fall asleep initially, alcohol aggressively disrupts your sleep cycle. It prevents you from entering REM sleep and often causes rebound wakefulness in the middle of the night. Limit alcohol consumption, and try to stop drinking at least three hours before bedtime.
7. Embrace Morning Sunlight
Light exposure is the strongest signal you can send to your circadian rhythm. When natural sunlight hits your eyes in the morning, it halts the production of melatonin and signals to your brain that the day has begun. This early morning light exposure acts as a timer, helping your brain release melatonin exactly 12 to 14 hours later. Make it a habit to step outside for 15 to 20 minutes within an hour of waking up. If you live in a gloomy climate, consider purchasing a sun lamp designed for light therapy.
8. Upgrade Your Sleep Gear on a Budget
A mattress that lacks proper support will aggravate joint pain and arthritis, making comfortable sleep impossible. You do not need to spend thousands of dollars on a luxury bed to see improvement. Adding a high-quality, three-inch memory foam mattress topper can instantly revitalize an aging, overly firm mattress for a fraction of the cost. Additionally, invest in a contoured cervical pillow if you suffer from neck pain. Proper spinal alignment reduces tossing and turning.
9. Stay Physically Active
Regular physical exercise deepens your sleep and helps tire out your body. Walking, swimming, and gentle strength training are excellent options for older adults. Be mindful of timing—vigorous exercise right before bed can leave you too energized to sleep, so aim to finish your workouts in the morning or early afternoon.
If you have a Medicare Advantage plan, check if it includes a fitness benefit like SilverSneakers. This program provides free access to thousands of participating gyms and community centers nationwide, making it easier than ever to stay active without straining your budget. You can find safe, senior-specific exercise routines through the National Council on Aging (NCOA).
10. Create a Calming Pre-Bed Routine
Your brain needs a runway to land. You cannot expect to watch a stressful evening news broadcast and immediately fall into a peaceful slumber. Dedicate the final hour of your day to relaxation. Turn off all screens—the blue light emitted by tablets and televisions tricks your brain into thinking it is still daytime. Instead, try reading a physical book, practicing gentle restorative stretching, or listening to an audiobook.
What Does Medicare Cover for Sleep Issues?
Navigating healthcare costs can be confusing, but Original Medicare provides excellent coverage for diagnosing and treating clinical sleep disorders. Below is a breakdown of how your benefits apply in 2026.
| Service or Treatment | Medicare Coverage Details | Your 2026 Out-of-Pocket Cost |
|---|---|---|
| Sleep Studies (Polysomnography) | Covered by Medicare Part B if you show clinical signs of sleep apnea. Covers Type I, II, III, and IV tests. | 20% of the Medicare-approved amount after meeting the $283 Part B deductible. |
| CPAP Machines | Covered by Part B as Durable Medical Equipment (DME). Starts with a 12-week trial period. | 20% of the approved rental cost after meeting the Part B deductible. |
| CPAP Supplies (Masks, Tubing) | Part B covers scheduled replacements (e.g., masks every 3 months, filters monthly). | 20% of the approved amount after meeting the Part B deductible. |
| Prescription Sleep Medications | Covered under Medicare Part D or a Medicare Advantage plan with drug coverage. | Varies widely based on your specific plan’s formulary, tier pricing, and copays. |
| Cognitive Behavioral Therapy (CBT-I) | Part B covers outpatient mental health services, including therapy for chronic insomnia. | 20% of the approved amount after meeting the Part B deductible. |

Costly Errors to Sidestep
When trying to solve sleep issues, well-meaning seniors often make mistakes that cost them money or jeopardize their healthcare benefits. Watch out for these common missteps:
- Buying a CPAP out of pocket prematurely: CPAP machines regularly cost between $500 and $1,200. Do not buy one with your own money before completing a Medicare-approved sleep study. If you follow the proper diagnostic steps, Medicare will shoulder 80% of the cost.
- Failing the Medicare CPAP compliance trial: Medicare will only continue to pay for your CPAP machine if you actually use it. During your initial 12-week trial, you must use the device for at least four hours a night on 70% of the nights. If you fail to meet this compliance standard, Medicare will stop paying, and the supplier may repossess the machine.
- Relying on over-the-counter sleep aids: Daily use of OTC sleep medications containing diphenhydramine (like Tylenol PM or ZzzQuil) can lead to morning grogginess, severe dry mouth, and an increased risk of falls. For safe, medically reviewed information on sleep aids, consult MedlinePlus.

When DIY Isn’t Enough
Lifestyle changes and bedroom upgrades work wonders for mild to moderate sleep disturbances. However, certain symptoms indicate an underlying medical condition that requires professional intervention. Schedule a prompt visit with your healthcare provider if you experience any of the following:
- You wake up choking, gasping for air, or your partner notices you stop breathing during the night.
- You feel an overwhelming, uncontrollable urge to move your legs when you lie down (a hallmark of Restless Legs Syndrome).
- You routinely fall asleep during the day while talking, eating, or driving.
- You act out your dreams physically by punching, kicking, or shouting while asleep.
Frequently Asked Questions
Does Medicare pay for a new mattress?
Under normal circumstances, Medicare does not cover the cost of a standard mattress. However, if your doctor prescribes a specific pressure-reducing mattress or an adjustable hospital bed to treat a documented medical condition, Medicare Part B may cover it as Durable Medical Equipment (DME). You will still be responsible for the 20% coinsurance after meeting your deductible.
How often will Medicare replace my CPAP supplies?
Medicare adheres to a strict replacement schedule to ensure your equipment remains hygienic and effective. Generally, you can get new disposable filters every month, new masks and tubing every three months, and a brand-new CPAP machine every five years, provided you still have a documented medical need for the therapy.
Is melatonin safe for seniors to take every night?
While melatonin is a naturally occurring hormone, taking it as a daily supplement can interact with blood thinners, diabetes medications, and immunosuppressants. Furthermore, many older adults take doses that are far too high, which can cause next-day drowsiness. Always consult your doctor before adding melatonin to your nightly routine.
Reclaiming your sleep requires patience and a willingness to adjust ingrained habits. Start by choosing just two or three strategies from this list to implement tonight. Whether it means setting a strict morning alarm, reviewing your prescriptions, or finally asking your doctor for a sleep study, taking proactive steps will lead you toward the restorative rest you deserve.
The information in this guide is meant for educational purposes. Your specific circumstances—including income, benefits, tax situation, and health needs—may require different approaches. When in doubt, consult a licensed financial advisor, tax professional, or healthcare provider.
Last updated: April 2026. Benefit amounts, tax rules, and program details change annually—verify current figures with official government sources.










