A single fall does not just threaten your physical independence; it can instantly derail your retirement budget. According to the Centers for Disease Control and Prevention (CDC), the medical cost of non-fatal falls among older adults reached a staggering $80 billion in 2020. While Medicare and Medicaid cover the majority of these expenses, older adults and their families still shoulder billions in private and out-of-pocket costs.
More than one in four Americans age 65 and older falls each year. However, falling is not an inevitable part of aging. Just as you diversify your investment portfolio to protect against market volatility, you can build your physical stability to protect against falls. By dedicating a few minutes each day to simple, evidence-based movements, you create a physical safety net that protects both your health and your life savings.
“The most important investment you can make is in yourself.” — Warren Buffett, CEO of Berkshire Hathaway
Investing in your physical strength yields guaranteed returns. We will explore seven highly effective balance exercises you can do right in your living room, break down how Medicare covers professional physical therapy, and highlight common mistakes to avoid so you can stay safely on your feet.

The Financial ROI of Fall Prevention
When assessing retirement expenses, most seniors worry about taxes, inflation, and prescription drug costs. Yet, mobility loss represents one of the largest hidden risks to your financial security. If you take a tumble and end up in the emergency room, the out-of-pocket exposure can be severe—especially if you rely solely on Original Medicare without a supplemental Medigap plan.
Consider the concrete numbers: the average treat-and-release emergency room visit for an older adult who fell unintentionally cost roughly $8,869 in 2021. If the fall requires hospitalization, those costs skyrocket. Prevention requires zero copays, zero deductibles, and no trips to a clinic.
| The Cost of a Fall | The Cost of Prevention |
|---|---|
| Medicare Part A hospital deductible (over $1,600 per benefit period) | $0 for at-home bodyweight exercises |
| 20% coinsurance for Part B outpatient physical therapy | $0 using household furniture for support |
| Thousands of dollars for home modifications (ramps, stairlifts) | $0 for developing natural core and leg strength |
| Potential cost of assisted living or 24-hour home care | 15 minutes of your time each day |
By treating exercise as a non-negotiable part of your financial and physical retirement plan, you proactively shield your assets from sudden medical shocks.

7 At-Home Balance Exercises to Protect Your Independence
Before you begin any exercise routine, prioritize safety. Wear flat, closed-toe shoes with non-slip soles. Set up your workout space near a kitchen counter or a sturdy, heavy dining chair so you can grab onto a solid surface if you feel unsteady. The National Council on Aging (NCOA) recommends the following functional exercises to strengthen your lower body and improve your equilibrium.
1. The Sit-to-Stand
This movement mimics the natural action of getting out of a chair, making it one of the most practical exercises for daily living. It strengthens your thighs, glutes, and core, which are the primary muscle groups that keep you upright.
- Sit near the edge of a sturdy chair with your feet flat on the floor, hip-width apart.
- Cross your arms over your chest. If you need assistance, rest your hands on the armrests.
- Lean your chest slightly forward and push through your heels to stand up straight.
- Pause at the top, then slowly lower your hips back down into the chair with control.
- Repeat this motion 10 times.
2. Single Leg Stance (The Flamingo)
Standing on one leg forces your brain and muscles to coordinate, improving your ankle stability and spatial awareness. This directly translates to better balance when walking or climbing stairs.
- Stand behind a sturdy chair and place both hands on the backrest.
- Slowly lift your right foot off the ground, bending your knee slightly.
- Hold this position for 10 to 15 seconds.
- Lower your right foot, then switch to your left leg.
- As you improve, try holding on with just one hand, then just one finger, and eventually hovering your hands just above the chair.
3. Heel-to-Toe Walk (The Tightrope)
This exercise narrows your base of support, forcing your core muscles to engage to keep you centered. It is highly effective for preventing sideways falls.
- Stand next to a wall or a long kitchen counter so you can trace your hand along it for safety.
- Step forward, placing the heel of your right foot directly in front of the toes of your left foot. They should be touching or almost touching.
- Step forward with your left foot, placing that heel directly in front of your right toes.
- Walk 10 to 15 steps down the line, keeping your gaze fixed on a spot straight ahead rather than looking down at your feet.
4. Sidestepping
We rarely practice moving side-to-side, yet many falls occur when we reach for something laterally or lose our footing while turning. Sidestepping builds strength in your hip abductors.
- Face a kitchen counter and lightly rest your hands on the edge.
- Keep your toes pointing straight ahead and your knees slightly bent.
- Step your right foot out to the side, then bring your left foot over to join it.
- Take 10 steps to the right, then reverse the motion and take 10 steps to the left.
5. Standing Heel Raises
Strong calves act as shock absorbers and help you push off the ground when walking. Weak calves often lead to shuffling, which dramatically increases the risk of tripping over rugs or thresholds.
- Stand tall behind your sturdy chair, holding on with both hands.
- Slowly lift both heels off the floor, rising up onto the balls of your feet.
- Hold the highest position for two seconds, feeling the stretch and contraction in your calves.
- Slowly lower your heels back to the floor. Do not let them slam down.
- Perform 10 to 15 repetitions.
6. Backwards Walking
Walking in reverse engages completely different muscle patterns than forward walking and heightens your sensory awareness. It is a fantastic way to sharpen your central nervous system’s response to unexpected movements.
- Stand next to a clear, straight wall or a long hallway counter. Place one hand on the wall.
- Look over your shoulder to ensure the path is clear.
- Slowly take a step backward with your right foot, landing toe-to-heel.
- Follow with your left foot.
- Take 10 steps backward, then turn around and walk normally to your starting point.
7. Assisted Forward Lunges
Lunges build immense power in the quadriceps and improve flexibility in the hips. This strength is crucial for catching yourself if you happen to trip forward.
- Stand next to a sturdy chair, holding on with one hand.
- Take a moderate step forward with your right foot.
- Keeping your torso upright, bend both knees slightly. Your front knee should not go past your toes.
- Push off your right foot to return to the starting position.
- Repeat 5 to 8 times on the right leg, then switch to the left leg.
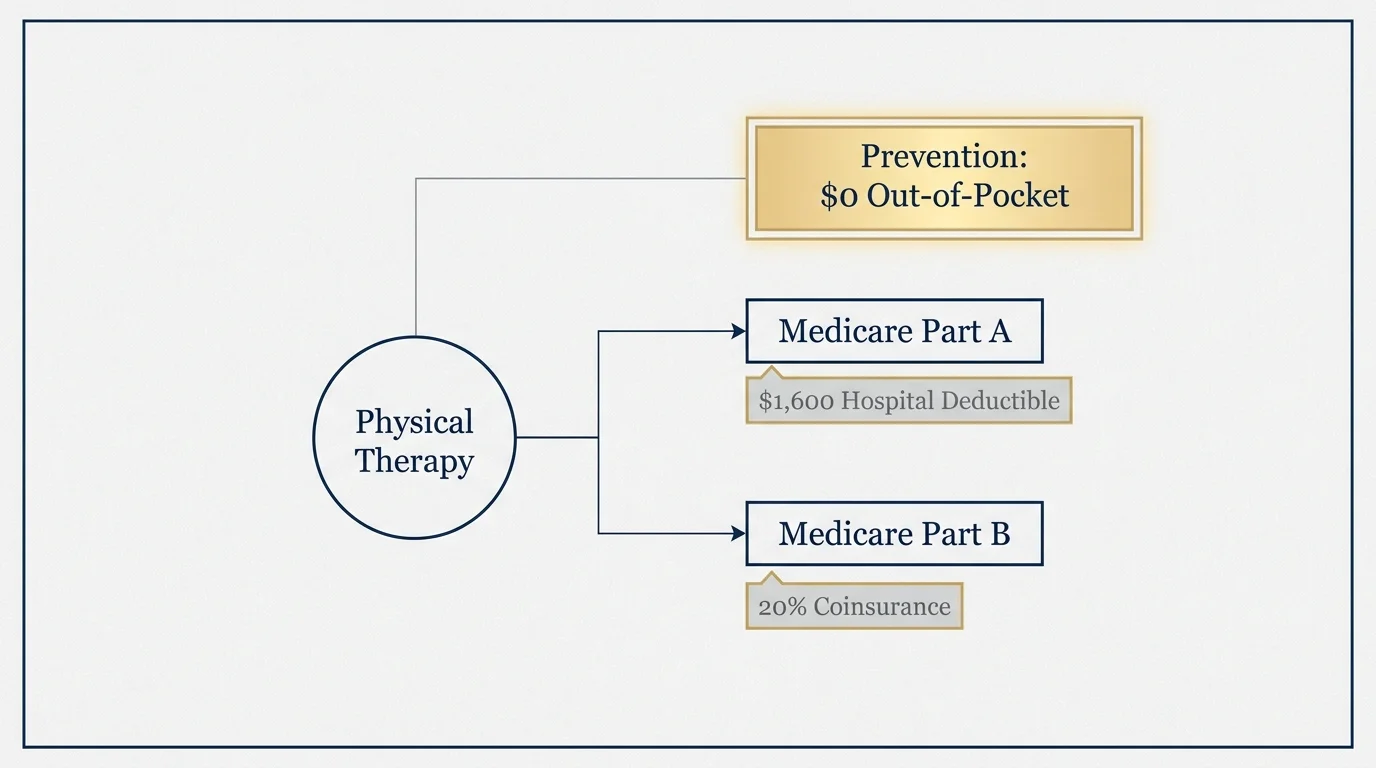
Does Medicare Cover Physical Therapy for Balance?
If you feel unsteady or have recently experienced a fall, at-home exercises might not be enough. You may need a personalized program designed by a professional. Fortunately, Original Medicare offers robust coverage for rehabilitation services.
Under Medicare Part B, medically necessary outpatient physical therapy is covered. In the past, Medicare enforced a strict financial cap on how much physical therapy you could receive in a calendar year. Congress removed this hard cap in 2018, ensuring seniors do not hit a dollar ceiling that halts their recovery.
Instead of a cap, Medicare uses a “therapy threshold.” Here is how the costs break down based on current 2025 limits:
- The Deductible: You must first meet your annual Part B deductible, which is $257 in 2025.
- The Coinsurance: Once the deductible is met, Medicare pays 80% of the approved amount, and you pay the remaining 20% coinsurance. If you have a Medigap plan (like Plan G), it generally covers this 20% gap completely.
- The Threshold: For 2025, the therapy threshold sits at $2,410. This is not a limit on your care; it is simply a documentation checkpoint. If your therapy charges exceed this amount, your physical therapist must formally document that continued treatment remains medically necessary for your condition.
Keep in mind that to qualify for coverage, your therapy must involve skilled services from a qualified professional. Medicare does not pay for general fitness training, but it readily covers neuromuscular re-education, balance training, and fall prevention protocols ordered by a doctor.
Pitfalls to Watch For
As you incorporate balance training into your routine, be mindful of these common mistakes that can inadvertently increase your risk of injury.
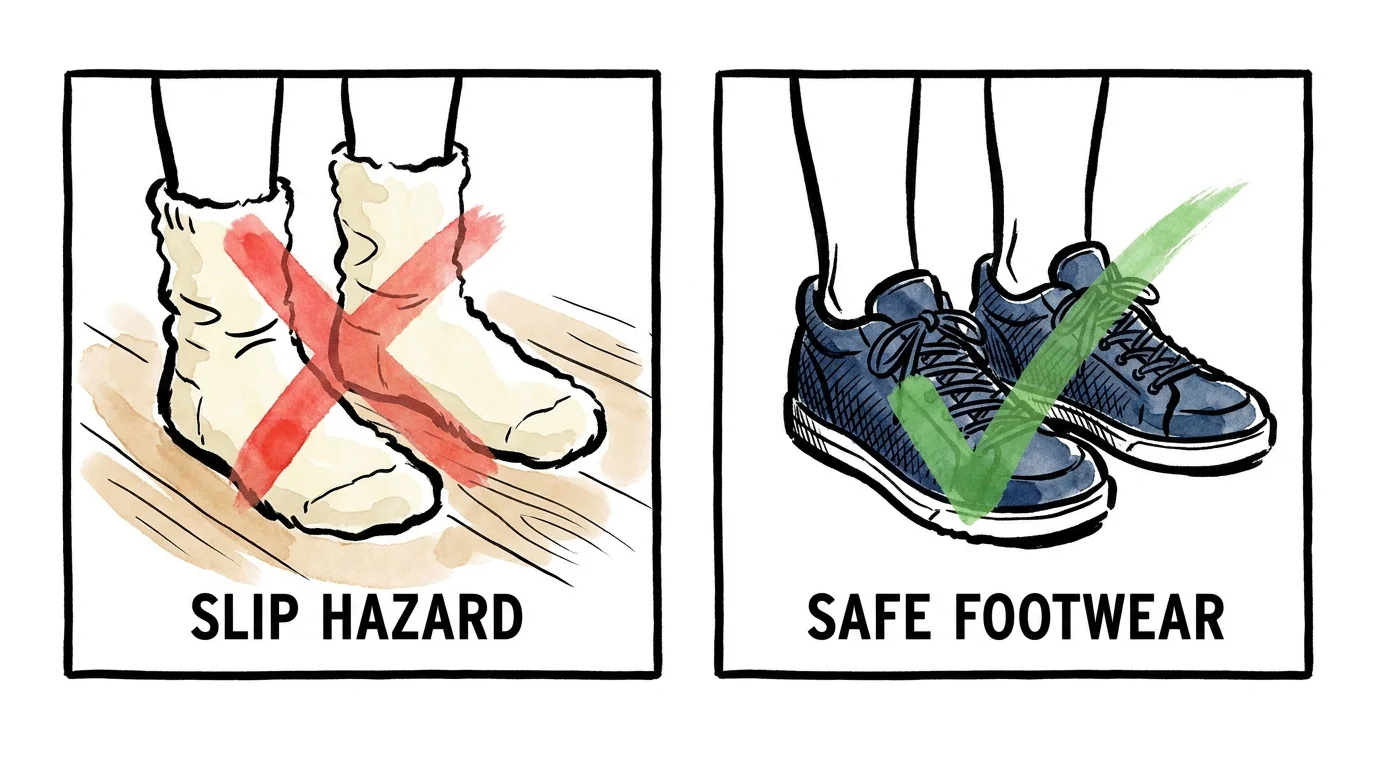
1. Exercising in Slippery Socks
Hardwood floors and wool socks are a dangerous combination. Always wear supportive, rubber-soled athletic shoes when performing balance exercises. If you prefer to be shoeless, invest in high-quality grip socks with silicone treads on the bottom.
2. Relying on Flimsy Furniture
Do not use a folding chair, a rolling office chair, or a lightweight TV tray as your balance support. These items can easily tip or slide if you put your full body weight on them. Always use a heavy dining chair, a locked wheelchair, or a built-in kitchen counter.
3. Keeping Falls a Secret
Less than half of older adults who fall tell their doctor about the incident. Many seniors fear that admitting to a fall will result in a loss of independence or pressure to move into assisted living. In reality, hiding a fall prevents your doctor from diagnosing underlying issues—such as medication side effects, inner ear infections, or vision changes—that can be easily corrected.
4. Pushing Through Sharp Pain
Balance exercises should challenge your muscles and make you feel slightly fatigued, but they should never cause sharp, shooting joint pain. If a movement hurts your knees or hips, stop immediately. Modify the depth of the exercise or consult a physical therapist for alternatives.

Getting Expert Help
Sometimes, the best financial and medical decision you can make is calling in a professional. Consider seeking expert guidance if you relate to any of the following scenarios:
- You experience dizziness or vertigo: Balance is not just about leg strength; it is heavily tied to your vestibular (inner ear) system. If the room spins when you stand up, you need an evaluation from a doctor or an Ear, Nose, and Throat (ENT) specialist.
- You catch your foot on the floor: If you frequently trip over thresholds or notice you are dragging your toes when you walk, a physical therapist can fit you for a subtle ankle-foot orthosis (AFO) to lift your foot automatically.
- You restrict your daily activities out of fear: If you have stopped gardening, attending social events, or going for walks because you are terrified of falling, look into community programs. The National Council on Aging supports an evidence-based program called “A Matter of Balance”. This 8-week structured group class helps older adults reduce their fear of falling, set realistic activity goals, and improve their coordination in a supportive environment.
Frequently Asked Questions
Does Medicare Advantage (Part C) cover balance classes?
Yes, Medicare Advantage plans must provide at least the same level of coverage as Original Medicare, meaning they cover medically necessary physical therapy. Additionally, many Part C plans offer supplemental fitness benefits—such as the SilverSneakers program—which provides free access to local gym classes focused on senior balance and stability.
Are there free fall prevention programs in my community?
Many local Area Agencies on Aging, YMCAs, and senior centers offer free or low-cost evidence-based programs. Look for classes like “Tai Chi for Arthritis and Fall Prevention” or “EnhanceFitness,” which are subsidized by state health departments and designed specifically for older adults. You can use the federal Eldercare Locator to find programs in your zip code.
How often should I do balance exercises?
For optimal results, aim to practice balance exercises three to four times a week. Consistency matters more than duration. Ten to fifteen minutes of focused, high-quality movement every other day will yield significantly better results than a single one-hour session on the weekend.
Taking the Next Step Toward Stability
Protecting your physical balance is one of the most proactive ways to safeguard your retirement. Every time you stand at the kitchen counter and practice a single-leg stance, you are actively defending your independence and keeping your hard-earned savings out of the emergency room. Start small, stay consistent, and do not hesitate to leverage your Medicare benefits if you need professional physical therapy.
The information in this guide is meant for educational purposes. Your specific circumstances—including income, benefits, tax situation, and health needs—may require different approaches. When in doubt, consult a licensed financial advisor, Medicare specialist, or medical professional.
Last updated: April 2026. Benefit amounts, tax rules, and program details change annually—verify current figures with official government sources.










