Maintaining physical coordination is one of the most effective ways to protect your retirement savings. Each year, one in four Americans over age 65 experiences a fall, leading to medical interventions that cost the healthcare system roughly $80 billion annually. While Medicare covers a significant portion, out-of-pocket costs for rehabilitation and home modifications can drain your nest egg rapidly. Assessing your balance early helps you identify potential mobility weaknesses before they result in an expensive injury. These seven simple, at-home coordination tests provide a practical baseline for your physical health. Performing them regularly helps you stay independent longer, ensuring your hard-earned money goes toward enjoying your retirement rather than paying for avoidable medical bills.
The Financial Reality of Physical Health
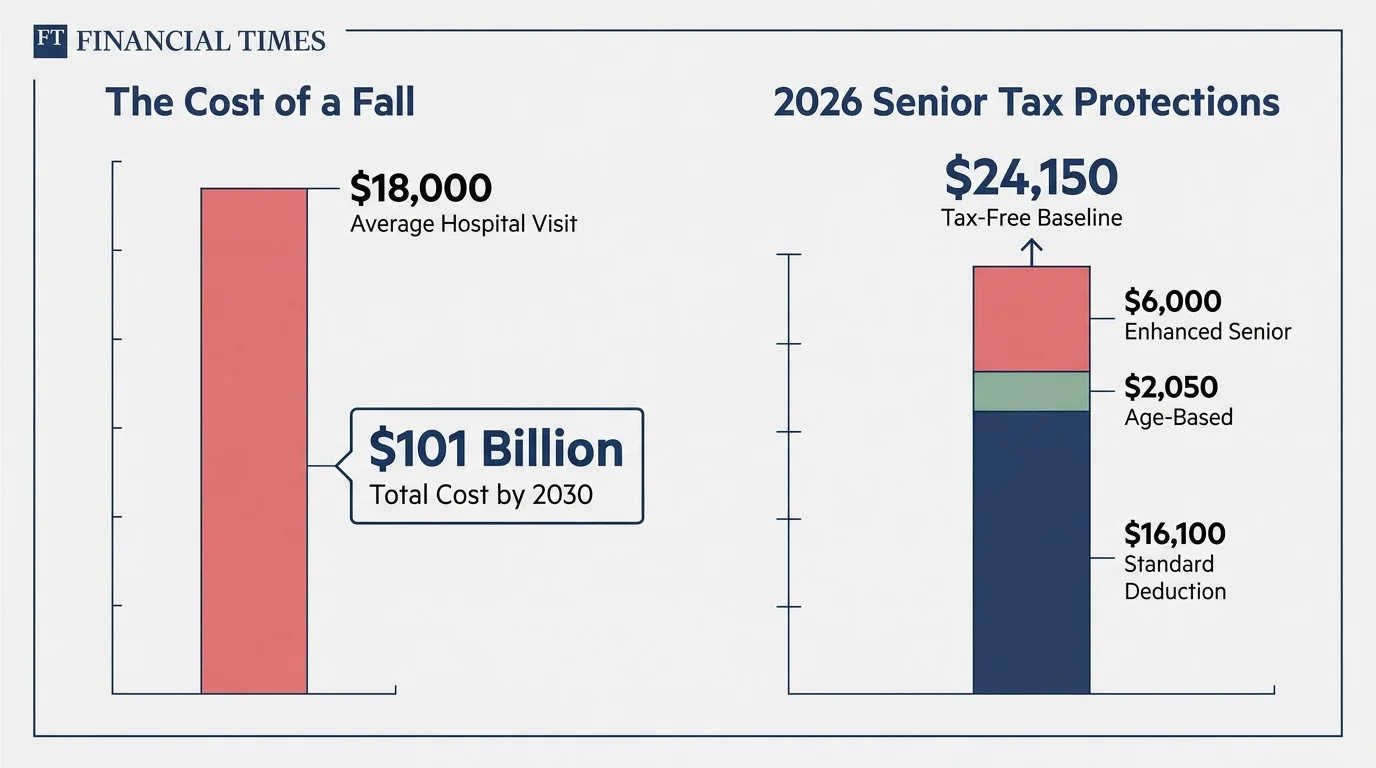
Aging in place comfortably requires both financial planning and physical maintenance. The National Council on Aging (NCOA) projects that treating fall-related injuries among older adults will climb to over $101 billion by 2030. When a fall occurs, the estimated average inpatient hospital visit costs more than $18,000. Medicare generally pays about 67% of these costs, but the remaining out-of-pocket expenses—copays, deductibles, private physical therapy, and necessary home renovations—fall directly on you.
Even favorable tax breaks cannot fully offset the financial shock of a major medical event. For instance, the IRS allows a single filer over 65 to claim a standard deduction of $16,100 in 2026, an additional $2,050 age-based deduction, and a new $6,000 enhanced senior deduction, bringing the potential tax-free baseline to $24,150. While these deductions help preserve your fixed income, spending thousands of dollars on preventable medical bills undoes much of that financial progress. Protecting your health is protecting your wealth.
“The greatest expense that we will all have moving forward is health care. Anything you can do now to reduce future health care costs is going to make whatever retirement savings you now have… last a whole lot longer.” — Jean Chatzky, Personal Finance Expert
Taking a few minutes every few months to check your physical coordination can keep you out of the hospital, lower your lifetime healthcare expenses, and preserve your financial independence.

Preparing for Your At-Home Assessment
Before you begin any physical assessment, prioritize your safety. The goal is to establish a baseline for your coordination and balance, not to push yourself to the point of exhaustion or injury. Treat these tests as a simple check-in with your body.
Set up your testing environment using these straightforward guidelines:
- Wear secure footwear: Perform these tests wearing flat, closed-toe shoes with non-slip soles. Avoid wearing just socks or backless slippers, as they drastically increase slipping risks.
- Use a sturdy chair: Use a solid, armless dining chair placed against a wall so it cannot slide backward. Avoid wheeled office chairs, plush recliners, or stools.
- Clear your space: Remove throw rugs, electrical cords, or low tables from your testing area to ensure you have a clear, flat surface to move across.
- Ensure adequate lighting: Turn on overhead lights so shadows do not distort your depth perception. If you normally wear prescription glasses, keep them on for the duration of the testing.
- Have a spotter: Ask a family member, friend, or neighbor to stand nearby. They do not need to hold you, but they should be close enough to catch you if you suddenly lose your balance.
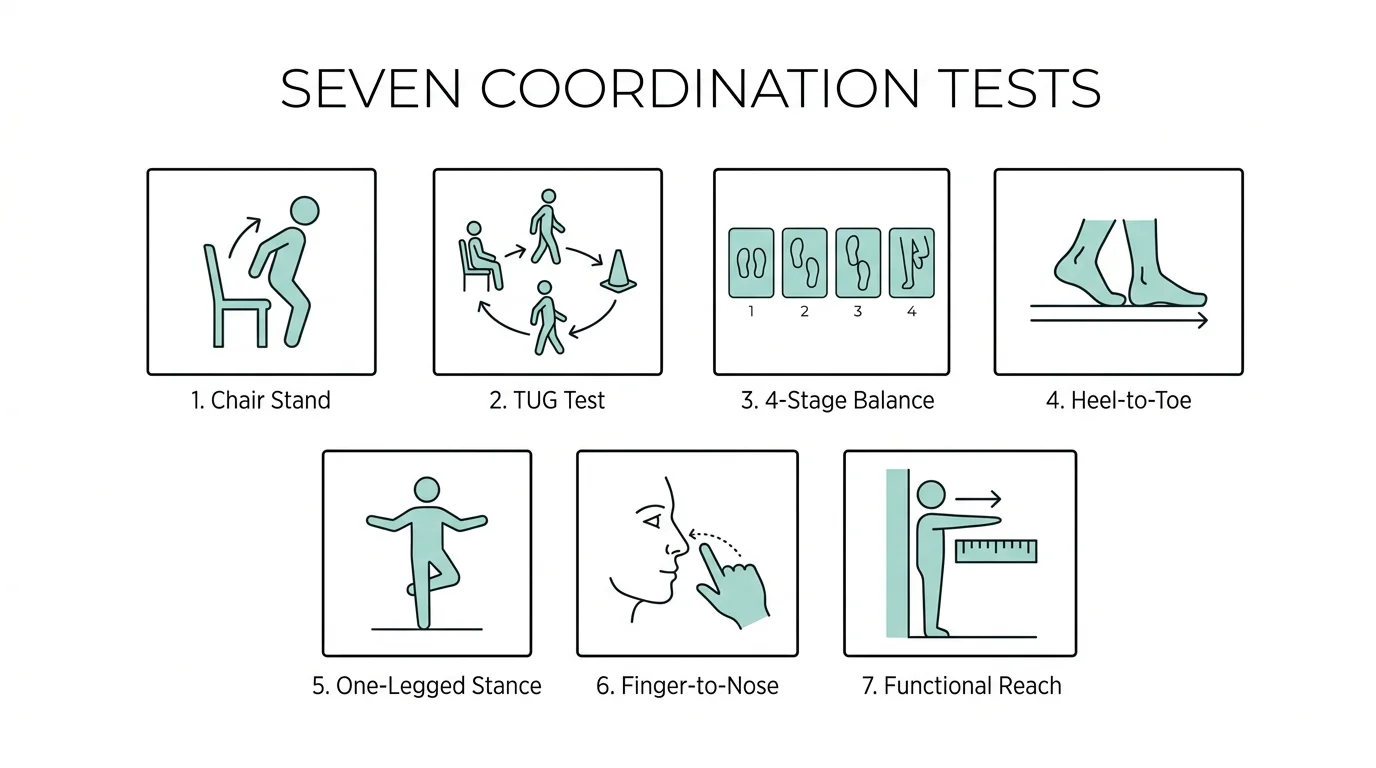
7 Coordination Tests Seniors Can Try At Home
The Centers for Disease Control and Prevention (CDC) developed the Stopping Elderly Accidents, Deaths & Injuries (STEADI) initiative to help healthcare providers safely assess fall risks. You can modify several of these clinical tests for at-home use to monitor your own mobility.

1. The 30-Second Chair Stand Test
This test evaluates lower body strength and endurance, which are vital for daily activities. If you cannot easily stand up from a chair, you may eventually struggle with getting out of a vehicle, rising from a soft couch, or managing personal hygiene independently. This translates directly into a loss of independence and a potential need for costly in-home caregiver assistance.
How to perform it: Sit in the middle of a sturdy chair with your feet flat on the floor and shoulder-width apart. Cross your arms over your chest, resting your hands on your opposite shoulders. Start a timer for 30 seconds. Stand up fully, then sit back down completely. Repeat this motion as many times as you safely can until the timer stops.
What to look for: Count how many full stands you complete. According to the CDC, a healthy target for someone between 65 and 69 years old is 12 or more stands for men and 11 or more for women. If you struggle to stand without using your hands to push off the armrests, it indicates a decline in leg strength that could compromise your overall balance.
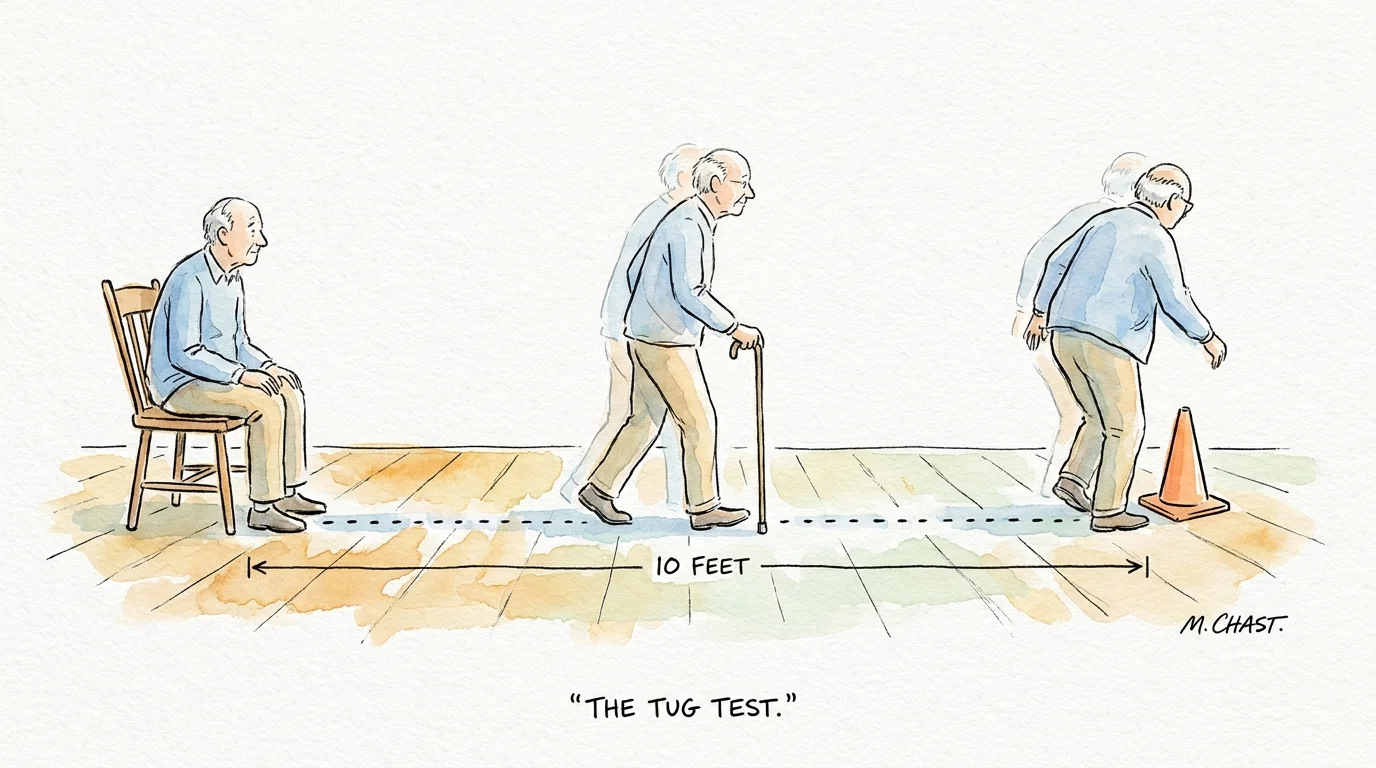
2. The Timed Up and Go (TUG) Test
The TUG test measures your functional mobility, agility, and dynamic balance—how well you move while changing speeds and directions. You use dynamic balance whenever you pivot to grab something off a counter or turn around to answer a ringing phone.
How to perform it: Place a piece of tape on the floor exactly 10 feet away from your sturdy chair. Sit in the chair with your back against the backrest. When your spotter says “go” and starts a stopwatch, stand up, walk at your normal, everyday pace to the tape on the floor, turn around, walk back to the chair, and sit down.
What to look for: Stop the timer the moment your backside touches the chair. Completing this test in 12 seconds or less is generally considered a healthy baseline. If it takes longer than 12 seconds, you may have an increased risk of falling and should discuss your mobility with a medical professional.

3. The 4-Stage Balance Test
This assessment checks your static balance in four progressively challenging positions. Do not move on to the next position unless you can hold the current one for 10 full seconds without stumbling.
How to perform it:
- Stand with your feet side-by-side, touching. Hold for 10 seconds.
- Place the instep of one foot so it touches the big toe of your other foot (a semi-tandem stance). Hold for 10 seconds.
- Place one foot directly in front of the other, heel touching toe (a full tandem stance). Hold for 10 seconds.
- Stand entirely on one foot. Hold for 10 seconds.
What to look for: You can hold your arms out to balance yourself, but you must not move your feet from their set position. An inability to hold the tandem stance (position three) for 10 seconds is a strong clinical indicator of increased fall risk.

4. The Heel-to-Toe Walk
Also known as tandem walking, this test checks your dynamic balance, spatial coordination, and proprioception (your brain’s ability to know where your body is in space).
How to perform it: Find a hallway or a room with a straight line—you can use the straight edge of a large rug or place a long strip of painter’s tape on the floor. Look straight ahead, not down at your feet. Place the heel of one foot directly in front of the toes of your other foot, so they touch or nearly touch. Take 10 to 15 steps forward in this manner.
What to look for: Notice if you constantly drift off the straight line, feel the immediate need to grab a wall, or have to step wide to catch your balance. Steady, controlled steps indicate good coordination.
5. The One-Legged Stance
This is a simpler variation of the final stage in the balance test, focusing entirely on unilateral stability. We rely on one-legged balance constantly without realizing it—every time you take a step, climb a stair, or step over a threshold, you are briefly balancing on one leg.
How to perform it: Stand near a wall or a sturdy kitchen counter so you can grab it if necessary. Lift one foot slightly off the ground, bending your knee. Keep your eyes open and look straight ahead. Time how long you can stand on one leg without holding onto a support surface. Switch legs and try again.
What to look for: While holding the stance for 10 seconds is a good baseline, holding it for 15 to 20 seconds shows excellent stability. A significant difference in balance between your left and right legs is a red flag worth mentioning to a physical therapist.

6. The Finger-to-Nose Test
Coordination involves more than just your lower body; upper body motor skills matter immensely, too. This test measures your fine motor coordination, depth perception, and neurological processing.
How to perform it: Sit comfortably in a chair. Extend both arms out to your sides, parallel to the floor. Keeping your eyes open, bring your right index finger in to touch the tip of your nose, then extend it back out. Repeat with your left index finger. Do this alternating motion three times with your eyes open. Then, close your eyes and repeat the alternating motion three more times.
What to look for: You should be able to smoothly and accurately touch your nose without hesitation or missing the target. Tremors, jerky movements, or consistently missing your nose—especially with your eyes closed—can indicate neurological changes rather than simple muscle weakness.
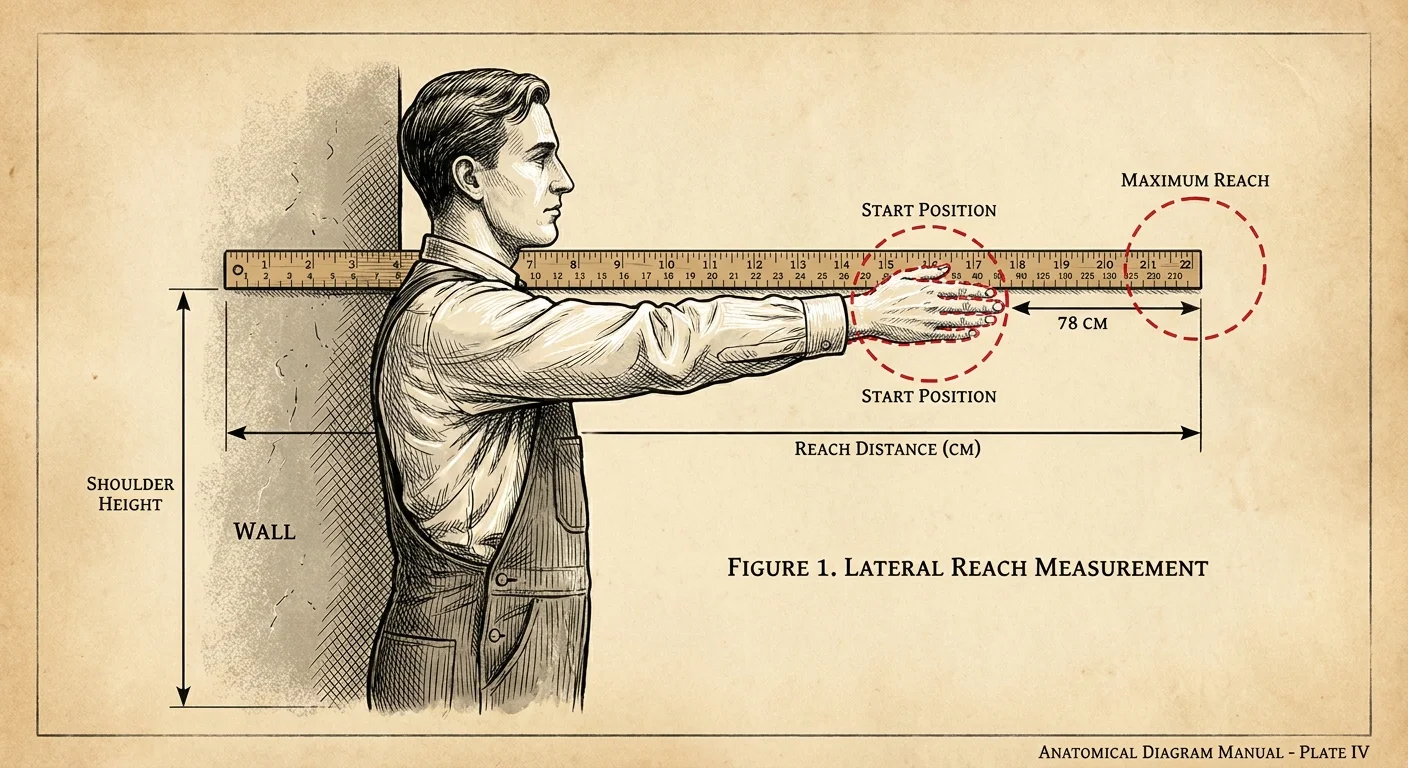
7. The Functional Reach Test
This test evaluates your balance while leaning forward, mimicking everyday tasks. Reaching forward without falling is required every time you grab a can of soup from the pantry, load the dishwasher, or pull mail out of your mailbox. Losing control of your center of gravity during these tasks often leads to sudden forward falls.
How to perform it: Stand with your side facing a wall. Raise the arm closest to the wall so it is parallel to the floor. Have your spotter mentally mark the wall where your fingertips end. Keep your feet flat on the floor and lean forward as far as you can without losing your balance or taking a step. Note the new position of your fingertips.
What to look for: Estimate the distance between the two marks. A reach of at least 10 inches is typical for a healthy older adult. A reach of less than 6 inches strongly suggests a risk for future falls due to a limited center of gravity control.
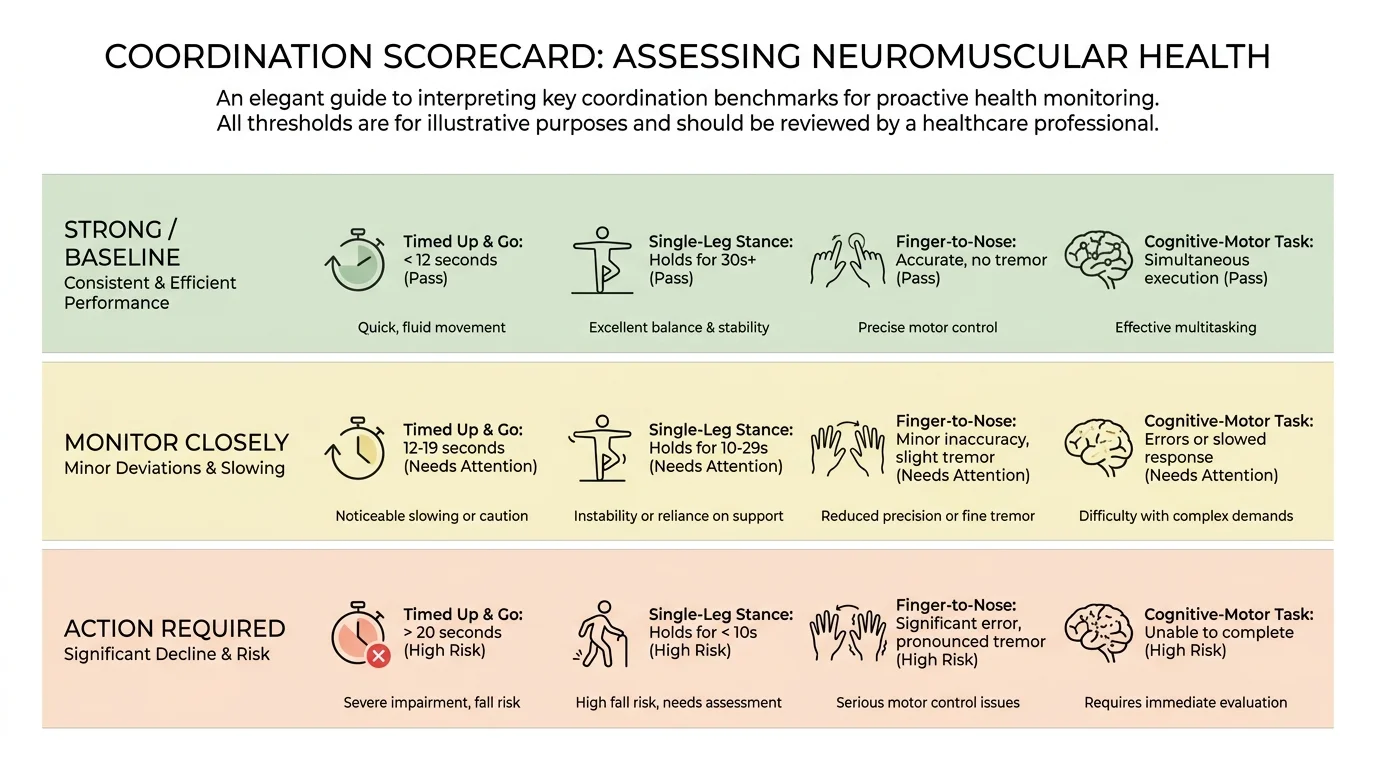
Understanding Your Results
Reviewing your performance across these different tests paints a comprehensive picture of your physical abilities. Use this chart to understand which areas of your mobility might need professional attention.
| Test Performed | Primary Skill Measured | Healthy Benchmark Indicator |
|---|---|---|
| 30-Second Chair Stand | Lower body strength and endurance | 11-12+ stands in 30 seconds |
| Timed Up and Go (TUG) | Dynamic balance and agility | Completing the course in under 12 seconds |
| 4-Stage Balance Test | Static balance | Holding the tandem stance for 10 seconds |
| Heel-to-Toe Walk | Spatial coordination | Walking 10 steps straight without stumbling |
| Functional Reach Test | Center of gravity control | Reaching 10 or more inches forward safely |

Common Mistakes to Avoid
Many seniors unknowingly compromise their safety or misinterpret their health status when evaluating their own mobility. Avoid these common pitfalls to protect both your physical health and your financial stability.
- Brushing off minor stumbles: A “near fall”—where you trip but catch yourself on a wall or piece of furniture—is a critical warning sign. Many people ignore these incidents because no injury occurred. Tracking your near falls provides valuable clues about declining coordination before a costly accident happens.
- Accepting poor balance as a normal part of aging: While our bodies change as we get older, losing your balance is not an inevitable or unfixable part of aging. Physical therapy, strength training, and balance exercises can rebuild your stability well into your 80s and 90s. Dismissing mobility issues prevents you from seeking interventions that are fully or partially covered by Medicare Part B.
- Failing to review medications: Certain prescription drugs—especially blood pressure medications, sedatives, and antidepressants—can cause dizziness or orthostatic hypotension (a sudden drop in blood pressure when standing). If you struggle with the chair stand or TUG tests, your medications might be the culprit. A pharmacist or doctor can review your prescriptions and potentially adjust dosages to improve your coordination.
- Wearing improper footwear at home: Many seniors walk around their homes in loose slippers or stocking feet. This drastically reduces traction on hardwood or tile floors. Invest in supportive, rubber-soled indoor shoes to prevent unnecessary slipping accidents.

Finding the Right Professional
Your test results dictate your next steps. Knowing who to consult ensures you get the right help while maximizing your insurance and financial benefits.
When to see a Primary Care Physician: If you experience sudden dizziness, miss your nose repeatedly during the finger-to-nose test, or fail to complete the TUG test in under 12 seconds, schedule a doctor’s appointment. They can evaluate underlying medical conditions, check for vitamin D deficiencies, and write a required medical referral for physical therapy.
When to see a Physical Therapist: If your lower body strength feels weak but you are otherwise healthy, a physical therapist can design a custom exercise program. Medicare Part B covers outpatient physical therapy when deemed medically necessary by a doctor, typically covering 80% of the Medicare-approved amount after you meet your Part B deductible.
When to see a Financial Advisor: If a recent health scare makes you realize your home needs permanent modifications—like a walk-in tub, grab bars, or a stairlift—a financial advisor can help you determine the most tax-efficient way to pay for them. They can review your long-term care insurance policy, manage retirement account withdrawals, or help you access home equity safely.
Frequently Asked Questions
Does Medicare pay for fall prevention programs?
Medicare Part B covers a yearly “Wellness” visit, during which your doctor will conduct a routine fall risk assessment. Based on the results, Medicare may cover physical therapy, mobility devices like walkers or canes, and even some community-based intervention programs. However, Medicare does not usually cover routine fitness center memberships, though Medicare Advantage (Part C) plans often include popular fitness benefits like SilverSneakers.
How often should I test my coordination at home?
Checking your balance every three to six months is a practical schedule. However, if you recently changed medications, received a new eyeglass prescription, or recovered from an acute illness, you should retest your coordination sooner to see if those changes impacted your stability.
Can I improve my coordination once it starts declining?
Yes. Balance and coordination respond remarkably well to consistent training. Evidence-based programs like Tai Chi, the Otago Exercise Program, and A Matter of Balance have been proven to reduce fall risks significantly. Ask your local Area Agency on Aging or senior center about subsidized classes in your community.
Are balance tests safe to do if I already use a cane?
If you rely on a cane or walker for daily mobility, do not attempt to perform tests like the one-legged stance or the 4-stage balance test at home without a physical therapist present. Instead, stick to supervised evaluations. An expert can safely assess your baseline while accommodating your need for an assistive device.
Taking a proactive approach to your health yields massive financial dividends. By setting aside 15 minutes to run through these simple coordination tests, you gain a clear understanding of your physical capabilities. Catching a decline in balance early allows you to address it with inexpensive physical therapy rather than facing a devastating hospital stay. Talk to your doctor about your results, investigate community fitness programs, and continue moving confidently through your retirement years.
The information in this guide is meant for educational purposes. Your specific circumstances—including income, benefits, tax situation, and health needs—may require different approaches. When in doubt, consult a licensed financial advisor or tax professional.
Last updated: May 2026. Benefit amounts, tax rules, and program details change annually—verify current figures with official government sources.










